The role of the veterinarian in promoting public health does not always involve work in developing countries or tropical places. Zoonotic diseases, or diseases common between animals and people, are present worldwide, including in the homes of pet owners.
It is clear that the importance of pets in today’s households is significant, and it is thus crucial for animal owners and physicians to take into account the pet when looking at disease dynamics in a family. Indeed, pets can serve as a source of infection to people, and vice versa, and the close contact that many have with their companion animals puts them at higher risk of infection from these pathogens. This is why the veterinarian should be an active member of a family’s health team and work together with family physicians when evaluating how the pets’ health can affect households.
In order to assess this risk of transmission of zoonosis from pets to humans, it is important to focus our attention on several groups who are at higher risk of infection. These usually include children, the elderly, pregnant women or those with depressed immune systems like those individuals with HIV, cancer or other chronic conditions.

Due to close contact with their pets, children are at higher risk of contracting diseases from companion animals. (http://leerburg.com/308.htm)
This does not mean that people should refrain from having pets and, if the animals are treated properly, the benefits of having a pet definitely outweigh the risks. What needs to be done is to realize that these animals should be maintained healthy in order to reduce likelihood of transmission of disease to people.
More than half of infectious diseases in people are shared with animals, including some of the more famous diseases like rabies, plague or influenza. However, there are more pathogens that pets can harbor and can infect people.
Roundworms & hookworms
Roundworms, specifically by Toxacara canis and Toxacara cati, are nematodes of the dog and cat that are commonly affect veterinary patients. Often seen in younger animals, toxacariasis is transmitted by ingestion of eggs from the environment or from contaminated

Child affected with ocular larva migrans from Toxacara infection (sunnysidevet.net)
meat, although nursing puppies an also acquire the parasite from the milk of an infected female. The disease in animals is usually mild and is characterized by gastrointestinal inflammation, distended abdomen and lack of weight gain. In some severe cases, worms migrating from the intestinal tracks to other organs such as liver or lungs can cause a more severe clinical appearance such as respiratory disease. Humans also get infected from ingestion of eggs from contaminated soil, or sometimes on animal’s fur. The parasite can also be present in larval form in tissues of a wide range of species such as cattle or birds, and as such, eating infected meat represents another transmission pathway. The disease in people is represented by two major processes: ocular-larva migrans and visceral-larva migrans. In ocular-larva migrans, parasites migrate to the eyes of the affected person, where they can generate strong inflammatory response. Visceral-larva migrans is characterized by larval migration to internal organs, where the parasite can become dormant. This disease is usually mild although inflammatory response can rarely lead to severe symptoms. In both of these syndromes, children are at higher risk of infection due to their close contact with dogs and cats as well as potentially contaminated soil or sand.

Cutaneous larva migrans from Ancylostoma infection. (ruby.fgcu.edu/courses/davidb/50249/web/clm1.htm)
Hookworms are also a common occurrence in veterinary patients. Caused by Ancylostoma or Uncinaria species, these infect dogs and cats, especially kittens and puppies as well as stray animals. Infected hosts shed eggs into the environment and the parasite needs to hatch and develop into a larva before becoming infective to other species. Disease in dogs and cats is usually mild and characterized by weight-loss and diarrhea however, severe infection can lead to anemia. One important characteristic of hookworms is that the larvae living in the environment have the ability to directly enter the skin or mucous membranes of hosts, which is how humans most commonly get infected. People walking barefoot outdoors can have hookworm larvae enter through the skin, causing intensely itchy and inflammed lesions where the parasite is seen migrating under the skin. Rarely, hookworms in people can cause pulmonary and gastrointestinal symptoms.
While hookworms and roundworms are some of the most common parasitic zoonoses of pets, it is important to remember that other parasites of dogs and cats can be transmitted to people, such as tapeworms (Dyplidium sp.) and whipworms (Trichuris sp.). In all these cases, frequent deworming of dogs and cats leads to a decreased chance of infection in people
Giardia
Giardia lamblia are unicellular protozoans that are present in both animals and people. Commonly found in the intestinal tract of many animal species including wildlife, the parasites are shed in the feces and can survive well in water sources. Clinical appearance in both animals and humans is similar, commonly showing gastrointestinal involvement. Dogs and cats most often have watery diarrhea that may be bloody, depending on the severity of the infection. Vomiting, lethargy and decreased appetite can also be present. Diagnostics is usually done through evaluation of a fecal sample by identifying the parasite its cyst form directly under the microscope, although other tests like ELISA can detect the microbe more efficiently. Humans show very similar symptoms, including diarrhea and abdominal pain. Treatment in both animals and people include medicating with drugs such as metronidazole or fenbendazole. In my experience, giardiasis in animals can be challenging to treat and using a single drug may not do the trick. The current recommended treatment includes using metronidazole and fenbendazole together for better control.

Stained Giardia protozoans in their trophozoite forms (cdc.gov)
It is important to recognize that, both in animals and people, the parasite can be present in asymptomatic individuals, which suggests that it is part of the natural flora. This means that those who show significant disease from an infection may be more sensitive to it, such as kids (and puppies) or the immune-compromised.
Finally, while Giardia is one of the most commonly recognized zoonotic diseases from pets, it is important to realize that, in practice, it may not be the most important. There are in fact several different strains of Giardia lamblia, and each strain commonly affects a specific host. For example, Giardia types C and D only infect dogs, while type F only infects cats – human infection from these strains is not likely to cause disease in people, who are usually colonized by type A2. Some strains, however can infect a wide range of species, including people, and those are the ones that have zoonotic potential.

Giardia Assemblages A1 and B are the only ones capable of zoonotic infection (Weese JS & Fulford MB. 2011).
Toxoplasma
Toxoplasmosis, caused by protozoan Toxoplasma gondii, is mainly a parasite of cats, however the it can be found in several other animal species and humans. The disease is generally mild in both animals and people and usually goes unnoticed in healthy individuals. As such, there can be a significant proportion of the population that has had previous infection and is therefore protected, as evidenced by their elevated blood antibodies to the protozoan. Cats are the primary reservoir for T. gondii and acquire the infection from feeding on raw diets or other animals such as rodents. In felids that are infected for the first time, a large number of oocysts can be shed in the environment and thus infect other animals and people if ingested. It is important to recognize that these oocysts take 1-5 days before being infective to other species but can survive in the environment, including water sources, for long periods of time.
Disease in both healthy cats and humans usually provides good lifelong immunity to further infection, however some cats can have short-lived diarrhea diarrhea and symptoms in people are usually non-specific including headache, fever and swollen lymph nodes. While infection in healthy individuals is generally asymptomatic, the issue with T. gondi arises when it is found in special populations, specifically pregnant women and the immune suppressed, where it can cause severe illness. Toxoplasmosis is a well-recognized disease that can affect foetal development leading to abortion and neonatal death, as well as neurologic signs later on in life such as blindness, deafness or mental retardation. While previous infection in women usually generates appropriate life-long protection against the disease, a previously uninfected pregnant woman will not be able to generate sufficient immunity to prevent toxoplasmosis in the foetus.
Likewise, the parasite can cause significant disease in those with depressed immune systems in people suffering from AIDS or undergoing chemotherapy, leading to symptoms such as encephalitis. Another important aspect of toxoplasmosis infection is the potential for latency, meaning that the parasite will become inactivated in organs of healthy individuals and remain embedded for the rest of their lives. Previously healthy people who become immunosuppressed can thus suffer from symptomatic toxoplasmosis from re-activation of these hidden cysts without the need for new exposure to the parasite.
Due to the possibility of severe disease in the population at-risk, some clinicians advocate for complete removal of cats in households of pregnant women or HIV-positive patients. This drastic measure can, however, be avoided by proper management of the pet cat as well as good hygiene. Proper hygiene habits are always mandated when dealing with animals, including pets, and frequent handwashing or avoiding contact with cat feces (especially 1-5 days old), but also dirt or sand, is essential. People at risk should refrain from handling cat feces if possible, however, if they are unable to do so, the use of gloves is definitely warranted, as well as washing litter box and utensils with warm water. Reflecting the situation in humans, immunosuppressed cats are at higher risk of disease, leading to longer oocyst shedding time, and maintaining a healthy pet is an integral part of disease management in people. Cats usually have a good habit of grooming themselves however, in unthrifty or ill animals, grooming may be reduced and the cats may carry more Toxoplasma oocysts on their fur. Keeping cats indoor is also a very good way to prevent infection, as they will not be exposed to rodents that may carry the protozoan. Since it takes a few days for the oocyst in cat feces to become infective, frequent, daily cleaning of the litter box is a very effective way to prevent human infection. Finally, it is interesting to notice that, although cat ownership has increased in the US, the incidence of toxoplasmosis as been decreasing.
Ringworm
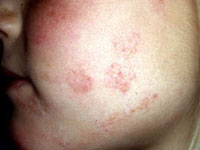
Ringworm (Microsporum canis) infection in a person. (dermnetnz.org)
Ringworm, or dermatophytosis, is one of the most common zoonotic diseases that affects a wide range of animals, especially cats, as well as people. It is caused by a group of fungus that can be found on the skin of many pets and can be spread to other individuals through direct contact, such as petting, but also fomites (couch, bedding) and fleas. Animals usually have a mild localized skin infection characterized by an area of hair loss and skin inflammation that may or may not be itchy. Likewise, in people, ringworm is characterized by circular skin lesions and is not usually severe if the individual’s immune system is working normally. Children tend to be at higher risk of infection due to their closer contact with pets. Not all cases of human ringworm are caused by a zoonotic species of fungus and it is important that physicians dealing with dermatophytosis infection in a family recommend veterinary examination of the pets to help control the outbreak.
Salmonella

Gram-negative staining of Salmonella sp. (textbookofbacteriology.net)
Salmonella are bacteria that are part of the intestinal flora of a wide range of animal species, especially cattle, and are mostly known as a food-borne pathogen. Symptoms in humans include diarrhea that can sometimes be severe and life-threatening. When it comes to pets, the traditional hosts of Salmonella include reptiles and birds and it is very important that people, and especially children, wash their hands after handling these animals. The bacteria are not common natural flora of dogs and cats and infection in these species usually doesn’t last more than a few weeks. In severe cases, gastrointestinal signs may occur. Therefore, the risk of transmission of Salmonella from dogs and cats to people is very low. This risk, however, can greatly increase in dogs and cats that are fed raw diets. I have seen from personal experience in the clinic that a significant number of people prefer to feed their pets raw diets. It is important to educate animal owners that these diets are usually not processed to the extent of other available pet foods and thus, contamination with bacteria such as Salmonella and E. coli will be transmitted to the pet. In fact, a study from 2008 has shown that dogs fed raw diet are 23 times more likely to shed Salmonella in their feces compared to dogs fed processed food, thus increasing chances of infecting people. This is why it is generally contraindicated to feed such diets, especially in households where there are people at higher risk of infection such as children or immunocompromised individuals.
Methicillin-resistant Staphylococcus aureus (MRSA)

Culture and antibiotics sensitivity testing is used to determine resistance in bacteria. Each dot represents a different antibiotic used; the clear area around each dot represents the degree of sensitivity to that specific antibiotic. (http://www.staph-infection-resources.com)
The rise of antibiotic-resistant bacteria has become an important issue in both human and veterinary medicine. Specifically, MRSA is a growing issue in human healthcare contexts such as hospitals. There are two recognized forms of MRSA infection in people: hospital-associated and community-associated. Staphylococcus aureus can be a common bacteria living in the upper respiratory tract and on the skin of humans. In healthy people, the bacteria generally does not cause disease, however, in people whose immune system is
depressed or skin is broken after a wound or surgery, MRSA can be the source of a significant infection. The challenge in the management of MRSA infections stems from the fact that the bacteria may be resistant to a wide range of antibiotics and, thus, treatment options can rapidly become limited.
S. aureus is not considered a common flora of dogs and cats, which are colonized by different staphylococcal species such as S. intermedius. Therefore, MRSA is usually not a natural occurrence in pets. The bacteria can, however, survive on the skin and nasal passages of household pets but colonization is usually self-limited and clears up on its own in about 14 days. In terms of disease in pets caused by MRSA, it is safe to assume that the same principles from human medicine apply and that the bacteria can be pathogenic in animals with wounds or depressed immune system. There is a consensus, however, that MRSA in animals is considered a reverse zoonosis, meaning that humans are the ones infecting pets. This is supported by the fact that, as previously mentioned, MRSA infection in pets is usually transient. Furthermore, studies have shown that dogs infected with MRSA reflect infection in the human population. This is significant because affected individuals can infect their pets, which can in turn re-infect their owners. This is the reason why collaboration between physicians and veterinarians is crucial when trying to get rid of an infection and thoroughly control MRSA in a household.
Human and animal health are intricately linked, and that may be even more apparent when it comes to companion animals. Most pet owning families share a close bond with their dogs and cats which can put them at greater risk of zoonotic infections, however this does not mean that they should give their animals away and not be exposed to the benefits of animal companionship. What needs to be done is to treat these pets as members of the family and thus provide them with appropriate care to ensure they remain healthy. The general guidelines to prevent transmission of zoonoses from pets to humans are very similar regardless of the diseases in questions: prevent pet contact with wildlife, frequent deworming, maintaining up-to-date vaccines and proper hygiene practices. Dealing with health problems in pets at an early stage is also more likely improve the animal’s health, reduce costs of treatment and decrease likelihood of transmission of disease to people.
Resources:
Rabinowitz PM & Conti LA. 2010. Human-Animal Medicine. Saunders Elseviers ed.
Weese JS & Fulford MB. 2011. Companion animal zoonoses. Blackwell Publishing.














































