For the past month, I have been working as a volunteer veterinarian at the American Fondouk, a mixed animal hospital in Fès, Morocco. The clinic offers free veterinary care to its patients and sees all sorts of animals from dogs and cats, to horses, donkeys, birds, sheep and goats. I chose this site to get more experience in promoting veterinary care in communities with limited resources as well as to see more public health-related cases.
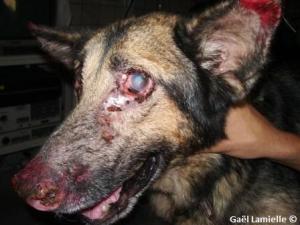
After a few weeks, I had the occasion to be exposed to such a case. The veterinary student externs were presented with an adult male German shepherd with recurrent epistaxis and crusting skin lesions on his face and ears. Upon closer examination, the lesions were distributed around the nose, eyes as well as the ear tips and were characterized by exfoliative dermatitis and ulceration. Ocular examination revealed bilateral anterior uveitis, keratitis and conjunctivitis.
Due to the history and clinical presentation, leishmaniasis was suspected. I scraped the affected area around the right eye using a scalpel blade to clear the debris until bleeding was noticed. I then made an impression smear of the bleeding lesion which was stained with Diff Quick. During microscopic evaluation of the sample, I noticed macrophages with intracytoplasmic structures characteristic of infection with Leishmania. The dog had previously been treated with allopurinol, with unfortunately no improvement and euthanasia was elected due to the poor prognosis.
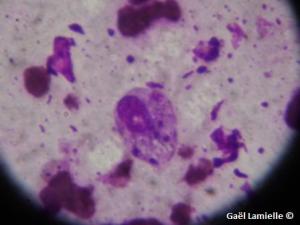
Macrophage from a direct smear of a periocular lesion. The intracytoplasmic inclusion bodies are consistent with Leishmania protozoans. (excuse the low quality of the picture…)
Leishmaniasis is a protozal disease seen in several different animal species as well as humans. It is distributed worldwide and affects millions of people each year. There are about 20 different species of Leishmania sp. and disease presentation can vary depending on the protozoan type.
Leishmania is present as a motile, flagellated protozoan in the vector, the sand fly (Phlebotomus & Lutzomyia), which feeds on mammalian hosts. As the parasite enters a host, it becomes non-motile and reproduces inside macrophages. The life cycle completes when another sand fly ingests a blood meal from an infected host. Wildlife reservoirs for the protozoan include rodents, hyaxes, dogs or foxes.

Life cycle of Leishmania sp. (http://www.dpd.cdc.gov/DPDx/html/Leishmaniasis.htm)
In North Africa, Phlebotomus sp. acts as the vector. However, in the United States, there have been reports of direct transmission, without the presence of an appropriate vector; direct transmission from a female dog to her pups has also been reported in the USA.

The Phlebotomus sand fly, vector of leishmaniasis in North Africa, is smaller than a mosquito and active throughout the night. (http://www.life-of-science.net/medicine/)
In animals, the disease is most commonly seen in dogs, although cats and horses can also show signs of infection. Canine leishmaniasis can have visceral, cutaneous and systemic component (although multiple forms can occur in a single animal). Clinical presentation is similar to the patient above and there is often cutaneous involvement. Other clinical signs present in dogs include anorexia, fever, lymphadenopathy and renal failure (the main cause of death in unmanaged cases). The disease in cats and horses is usually milder and is characterized by non-healing ulcers on the ear tips or muzzle.
Treatment in dogs is often unrewarding and no good protocol has been found yet. Common medications used include allopurinol or Pentostam (sodium stibogluconate). Even well-managed patients can show high rates of recurrence.
Human disease also varies in clinical appearance. Cutaneous manifestations can be simple or diffuse and are usually characterized by nodules on exposed areas of skin (most often face & hands), which can develop to ulcers. Simple cutaneous infection is often self-limiting while the diffuse form can be lifelong. Symptoms of visceral leishmaniasis in people (Kala-azar) include weight loss, fever, splenomegaly and hepatomegaly. Once again, the illness can resolve on its own, however, in immunocompromised or malnourished individuals, the disease can be fatal. Resolution of the visceral form can also be followed by the cutaneous form. Mucocutaneous leishmaniasis is a more aggressive form found primarily in Latin America and is characterized by erosion of the nose or oropharynx.
Treatment in people is often long and depends on the form of the disease, geographical location and species of Leishmania. Pentostam and meglumine are often used; guidelines from the World Health Organization (WHO) also include the use of amphotericin for visceral leishmaniasis.
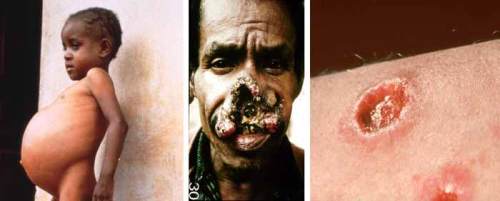
From left to right: visceral, mucocutaneous & cutaneous leishmaniasis. (http://wiz2.pharm.wayne.edu/module/antiparasitic.html)
Infection rates in people and animals are increasing worldwide and it is important to look to environmental factors to explain this trend from a One Health perspective. Some of these factors include increased human-wildlife contact, such as in newly deforested areas where populations have increased contacts with sand flies. Another theory that has been put forth regarding many arthropod-transmitted diseases is global warming. As average summer temperatures rise, vectors find more suitable environments and establish persistent populations at higher latitudes.
For more information on Leishmaniasis:
Leishmaniasis – Iwoa State Center for Food Security and Public Health
Rabinowitz PM & Conti LA. 2010. Human-Animal Medicine. Saunders Elseviers ed.

Nice post Gael. Thanks for sharing your experience in Morocco with us.
By: ychou on September 12, 2011
at 17:29
[…] and brought to Los Angeles, where it was was diagnosed with leishmaniasis (see previous post: Working in Morocco – Recurring leishmaniasis in a canine patient). This is a disease that is not established in Los Angeles and dogs need to be on lifelong […]
By: Dog imports into the United States | Global Health Vet - A One Health approach to public health on October 31, 2014
at 02:09